STIgma: STIs and the city
Hands up: who has ever been hunched over a hand mirror with their legs spread, panicking about something burning, itching, stinging or just feeling not quite right in their pants? Hello? Anyone?
Sexually transmitted infections are stigmatised in Australia, creating a wealth of problems for both the individuals diagnosed with them and broader society. It’s similar to the stigma surrounding mental health, but unlike what’s happening in our mind, we are less likely to talk about what’s happening in our pants. It’s also highly unlikely the ABC will broadcast a variety show dedicated to STIs. But why?
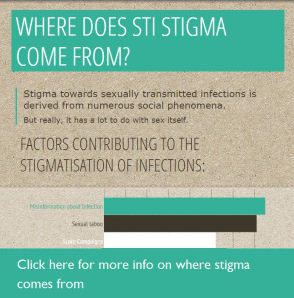
The social phenomenon of STI stigma stems from multiple factors. What is obvious – based on information from doctors, academics and people living with or without an STI – is that both misinformation about infections, as well as the ravages of millennia-old sexual taboos, play a huge part in how we conceptualise STIs.
In our privileged first world nation, all STIs are treatable, from curable gonorrhoea to the chronic infection of herpes. Modern medicine has progressed to the point where even the much maligned human immunodeficiency virus – HIV – is being reconceptualised by health professionals. Family Planning NSW Medical and Clinical Services Director, Dr Deborah Bateson says the virus is now a lifelong condition rather than a stepping stone on the path to an AIDS grave.
‘Now we’re looking at how people manage conditions of old age with HIV,’ she said. Once people learn of such health outcomes, it appears stigma is less so from the threat of serious illness and more derived from the social construction of a sexual hierarchy.
The idea of “dirty” sex became a part of our identity as soon as the First Fleet touched down on Australian soil. We are still following in the footprints of their European, Judeo-Christian culture, despite many of us distancing ourselves from organised religion. Associate Professor of Theology at the University of Newcastle, Dr Roland Boer says the Christian Bible lays out a number of rules controlling peoples’ bodies and sexuality that are still with us today.
In the Bible, Leviticus and Corinthians govern some reproductive functions with banishment from the tribe, as well as chastise “sexual immorality” and valorise “self-control”. From these passages, it’s evident the notion of “uncleanliness” still shapes how we perceive STIs today.
‘The basic point is that religious institutions and the cultural traditions that stem from them in “secularised” societies have trouble dealing with sex,’ Dr Boer said. ‘That is the core issue, which then has ramifications for their approaches to STIs.’
When we look at genital herpes, we can see how sexual taboo and misinformation play up the anxiety surrounding infections. Have you had chickenpox, shingles, glandular fever or a cold sore? Well, you have had one (or more) form of herpes. The virus family seems to be tolerated when it is anywhere but in our underwear. Kate was diagnosed with herpes 15 years ago and says the ongoing stigma she has experienced is all down to sexual taboo. ‘That [genital] area is considered “clean” or “dirty”,’ she said. ‘They’re very, very personal – those parts of our bodies. It’s got lots to do with sex, really.’
Stigma at the macro level
Historian and University of Newcastle lecturer, Dr Lisa Featherstone has conducted extensive research into sexuality in Australian society. Over the course of the 20th Century, she says we have not seen progress in our understanding of STIs and sexual taboo, ‘so much as a history of moving forward [with] small steps backwards’. Sexual taboo has morphed from curbing extramarital pregnancy, to largely focusing on body policing.
‘The white male heterosexual body is [considered] a normative body… if you sit outside of that then your body might be problematic in some way,’ Dr Featherstone said, pointing out this includes contracting an STI.
In some cases, “problematic” bodies have resulted in extreme government policy. In the early 20th Century, Australian working class women were subjected to compulsory vaginal exams for syphilis. The government’s right to do this was enshrined in law. If women refused they were jailed. If they were found to have syphilis, they were treated and, Dr Featherstone says, also detained over the course of medical intervention. Of course, these days syphilis is a curable infection.
While such government control has died off – to an extent – it can be seen as one of the more formalised symptoms of STI stigma. When we consider current legislation regarding disclosure of HIV status, we see modern issues of institutionalised stigma for people living with infection. State by state, public health and criminal laws differ on the matter. In New South Wales, failing to either alert a partner of your positive diagnosis or take reasonable precautions to avoid passing on the infectioncould land you in jail. This raises the question: one day, if there is a cure for HIV, will we relate these laws to the human rights abuses afforded women suspected of having syphilis?
Sexual taboo inhibits discussion of STIs as we believe there is a type of person who catches them. Ever seen the film Philadelphia? Protagonist Andy is embroiled in a legal battle for his unfair dismissal on the basis of his HIV/AIDS status. In his employer’s defence, a lawyer implies Andy somehow deserved to catch HIV as a promiscuous gay man, contrasting him with a female employee who contracted HIV through a blood transfusion during childbirth. More than 20 years since Philadelphia’s release, these judgements are still with us – both in media and on the street – as we prescribe blame to sexual behaviours operating outside formalised heterosexual unions.
While – statistically speaking – there are lifestyle factors and choices that may increase your risk of contracting an STI, viruses and bacteria are not judges of character. An STI will set upon anyone who bleeds red. Dr Bateson says there are a lot of misconceptions about who can contract an STI.
‘They do not discriminate on the basis of age… where you come from, of socioeconomic class,’ she said. ‘People of all different backgrounds can catch an STI.’
This proves to be the case for a number of people living with genital herpes. Kate believes she contracted the virus from her long term partner when he returned home after six months abroad. In testament of Dr Bateson’s hypothesis, Damien says he caught herpes quite early on in life.
‘As a boy, I was always very excited about my first real girlfriend… so catching genital herpes at the same time as losing my virginity was absolutely horrible,’ he said. ‘Sex is a huge part of our lives and… as a guy, having a disease [sic] on the most important tool I will ever own kind of always made me feel dirty and fearful that others would feel the same.’
Indeed, it is possible not to have engaged in consensual sex and be living with an STI. People surviving sexual assault are not immune to STIs. Furthermore, a number of infections, including HIV, herpes and warts, can be passed on to children during conception or birth.
Experiencing stigma: the micro level
Social stigma is the main issue for those who are diagnosed with STIs – especially those infections that are for life and not just Christmas while their regular doctor is on holiday. Medical professionals say diagnoses are common. For the people living with chronic STIs, however, they feel isolated because few people want to share their experiences.
Adrian has been living with HIV since 1992. In this time, he has not been able to disclose his STI status in all facets of life because, for the most part, Australians ‘are still stuck in the mindset of it being a killer disease’. He says society has not yet become accepting of what HIV now is, in comparison to how he feels able to inform people he identifies as a gay man.
‘When you’re diagnosed with HIV, it’s a lot more than coming to terms with a medical condition,’ he said. ‘Basically, you take on all that is associated with HIV and AIDS. The stigma, initially, comes in the form of a huge weight.’
This is a truism for a number of STIs. The sheer mass of stigma bears down on interactions with family and friends. Adrian says people can become labelled by their STI status.
‘You run the risk of becoming the person with HIV, rather than the person who plays the guitar or the person who writes books,’ he said of weighing up whether to disclose his status to someone.
Of course, sexual relationships are massively affected by STIs. Dr Bateson says for the majority of people, the anxiety associated with their infection is less about them and more to do with how prospective partners will perceive them. For curable STIs, anonymous apps help to inform partners of potential exposure to an infection. For people with a chronic infection, the process is ongoing and more often face to face.
‘Often there’s fear around transmitting it to someone else and fear about starting a new relationship,’ she said.
As a newly single mother at the time of her diagnosis, Kate seemed to experience all these levels of social stigma at once. Her friends would make snide comments about herpes and she would have to bear it without a sound. They would try to set her up with friends in spite of her refusals. She felt unable to disclose her “reality” to anyone and was celibate for seven years.
‘I just put all that part of my life: my own sexuality, my own expression – and I’m quite an expressive person… under a table and [made] it non-existent,’ she said.
Kate has come to grips with her STI and is back on the dating scene. Unfortunately, not everyone is at this level and Kate explains the perils of “the talk” – informing a prospective lover of your diagnosis – can be draining on one’s morale and libido.
‘I have met some seriously, seriously broken people because of this… that are just crushed, they’re absolutely hopeless about it,’ Kate said, noting many people experience ongoing rejection.
To alleviate some of the difficulties in finding love – or a quick hook-up – with an STI, online services have provided options to navigate the talk. They can potentially eliminate the talk if utilising services set up especially for people with STIs. Ultimately, they can prove expensive, limit a person’s options, and discrimination is just as readily felt in this environment as in the physical world. Ever seen the troubling phrases ‘drug and disease free’ or ‘are you clean?’ bandied about?
Stigma affects us all
The challenges faced by Kate, Adrian and the many Australians diagnosed with an STI may prompt safer sex practices. Stigma, however, has a negative impact on infection prevention. Frankly, you would be doing well to have pulled out a looking glass and examined your nether regions once in your life.
Two out of five people surveyed for this article feel STI stigma prevents them getting tested for an STI or chatting with a clinician.
‘I do hear people say “I don’t want to get tested, I just don’t want to know because I’d get really anxious and upset if I knew”,’ Dr Bateson said. ‘People do fear what the tests are going to show and we need to show them, actually, that STIs are very common.’
Almost one in three say stigma stops them discussing safer sex and STIs with partners, with 31% feeling unable to inform partners of a diagnosis.
‘Because it’s sexual, people don’t want to talk about it, they don’t want to know about it, they don’t care – until it hits them,’ herpes advocate and co-author of The Living Sphere Guide to Herpes, Jeannie May said. Jeannie, along with many people living with an STI, believes denial is easier for some. In this culture of stigma, the population seems to drop their pants, place a finger in each ear, close their eyes tightly and shriek to avoid any knowledge of STIs. Very kinky.
For those affected by STIs, they feel there’s still a long way to come in terms of balancing sexual health promotion in both medicine and media with preventing stigma. ‘It is important that people are aware of STIs and the risks,’ Jeannie said. ‘Unfortunately, awareness campaigns reinforce the perception that STIs are something you really don’t want to get.’
The Australian medical community has come a long way since the 1980s Grim Reaper advertising scare campaign for HIV/AIDS, or previous interventions it had to stage on behalf of the government to end syphilis. Sexual health bodies now see the importance of the balance Jeannie speaks of. Dr Bateson says Family Planning acknowledges the majority of people are libidinous and the organisation wants them to enjoy sex.
‘We don’t want people to feel stigmatised, but we want them able to prevent STIs where they can,’ she said. ‘If they do contract an STI we want to be able to manage that in a sensitive way, where they feel empowered.’ Until there’s a cure, people touched by chronic STIs wait for the rest of us to catch up with this view.